The aim is to promote a safer intervention in a cardiac arrest assisted by a sports professional during the current pandemic conditions due to COVID-19. The European Resuscitation Council protocol for lay people is adequate for this group, but it must be complemented with the use of personal protective equipment (PPE) adapted to sports professionals. The adaptations of action with respect to the 2015 practical guidelines are: assessment of breathing visually without opening the victim's airways, placement of a mask (preferably>FFP2) on the victim before starting resuscitation, resuscitation only with chest compressions except for of children and drowned-cohabitant, and the use of PPE for the sports field of easy learning and greater safety against possible transmission of COVID-19 by drops/aerosols (FFP3, glasses, gloves). These considerations should be included in the training/re-training of sports professionals in resuscitation and sports entities should favour the availability of aforementioned PPE.
The sports sector is not risk-free, even though physical activity provides indisputable health benefits, at the same time high intensity exercise may increase the risk of acute cardiac events.1 Sudden death affects mostly athletes who are older than 35 years of age and the cause is usually coronary artery disease, while young athletes have a lower incidence (2 every 100,000) and the cause is usually congenital/inherited.1 Some unfortunate sudden deaths are well known in professional sports because of its impact on the media and the tragic deaths of football players like Antonio Puerta and Dani Jarque.2
In the case of sudden cardiac death when an athlete is training or competing in an out-of-hospital environment, it will be key that people who are around (coaches, physical trainers, other athletes, healthcare professionals, etc.) can identify the emergency and react properly to increase the survival rate and improve the victim's prognosis. It is worth mentioning that CPR, when performed immediately after sudden death strikes, can even quadruple the victim's chances of survival.3 That is why it is essential to have a basic first aid knowledge, including basic life support (BLS) as well as training the skills to perform cardiopulmonary resuscitation (RCP) and defibrillation.4,5
At the end of 2019, the severe acute respiratory syndrome (SARS-CoV-2) that causes coronavirus disease 2019 (COVID-19) emerged.6 Currently, we are still in the midst of a global pandemic, which was declared by the World Health Organization (WHO) on March 11, 2020.6 Due to its high contagiousness, especially through aerosols, different measures have been promoted to prevent the spread of the virus. Population has generally been advised to keep interpersonal distancing, wear face masks and wash hands with water and soap or hydroalcoholic gel.7 In the field of sport there have also been preventive measures recommended to keep a safer practice, including limiting attendance, improving indoor ventilation and increasing interpersonal distance.8,9 In case of cardiac arrest, due to the fact that keeping interpersonal distance between rescuer and victim is impossible, the European Resuscitation Council (ERC) has adapted the guidelines for cardiopulmonary resuscitation performance in coexistence with COVID-19.10 These adaptations aim at providing safety for rescuers when there is a victim with suspected COVID-19 and concern healthcare professionals as well as lay health workers. These recommendations together with other scientific evidence are going to be analyzed to see which changes apply to rescuers in the field of sports. If a sports professional treats a victim of sudden death who could be infected with COVID-19, the sports professional must be aware of the following adaptations based on scientific evidence: safety before and after the intervention, assessment of the victim, CPR, use of defibrillation, use of personal protective equipment and BLS. With regard to this I propose the following objective.
ObjectiveThis paper, in accordance with the current knowledge, aims at promoting a safer performance in case of sudden cardiac arrest when performed by a professional of the sports sector during the current conditions of the COVID-19 pandemic.
Basic life support and defibrillation in the sports sector during the COVID-19 pandemicSafety before interventionBefore intervention in case of sudden death, the environment must be taken into account to minimize the transmission of droplets/aerosols. To do so, if the cardiorespiratory arrest occurs indoors (for example, volleyball court, changing rooms, etc.), windows and doors must be opened to improve ventilation during the intervention.11 However, if the event occurs outdoors in windy conditions,12 it would be a good choice for the rescuer to stand next to the victim at the side where the wind does not blow directly into the rescuer face (from mouth/nose of the victim).
Assessment of the victimA victim is having a cardiorespiratory arrest when there is not responsiveness and breathing is not normal. In order to determine whether the victim has consciousness in coexistence with COVID-19, the procedure is still the same, the rescuer will smoothly shake the victim's shoulders while speaking to them loudly.5 However, when assessing breathing, the procedure has been adapted to favour the rescuer's safety. Breathing will be visually assessed without opening the airway from the victim and the rescuer will not need to approach the victim's mouth/nose.10,13
Cardiopulmonary resuscitationBefore starting CPR, it is recommended to place a covering over the victim's mouth/nose.10,13 A towel or a piece of cloth can be used for this,10,13 or preferably a N95 face mask.14 During chest compression, passive ventilation takes place15 and it can generate droplets/aerosols in the same way as it occurs during chest compressions in physiotherapy techniques.16 N95-FFP2 face mask is more filtering to protect against droplets/aerosols than the surgical mask or than wearing no mask.14
Rescue ventilations will only be performed by emergency professionals or by trained healthcare professionals with personal protective equipment (PPE) against aerosols and appropriate ventilation devices.10,13,17 Regarding cardiac arrest, sport professionals should not perform rescue ventilations even if they are trained.
In general, hands-only CPR (only compressions without ventilations) together with the use of defibrillator is validated as a good option for the most of sudden death events in sports during the COVID-19 pandemic. This is because it is usually attributed to heart conditions. Exceptionally, it could be accepted that a sports professional performs rescue ventilations, only if they are trained and able to confront two situations in which fighting hypoxia is crucial. One situation would be if the victim is a child10,13 and the other situation would be if the victim is a drowning person and victim-rescuer belong to the same household.18
DefibrillationDefibrillation will be done as suggested by the 2015 guidelines,5 because it is unlikely that this procedure presents additional risks due to aerosols generation. Given that adhesive pads can be placed without direct contact between rescuer and victim, defibrillation is thus considered a safe practice.10
Post-interventionAfter intervention, it is recommended that rescuers wash their hands correctly and contact the health authorities.10,13 Handwashing with alcohol gel or water and soap is recommended to kill COVID-19.7,19 In addition, the rescuer's clothing as well as all the elements that have been used during the intervention should be removed, since they might contain aerosols generated by the victim. When taking off clothing, a face mask must still be worn and contact with eyes must be avoided. Finally, the rescuer's mask must be replaced with a new one and hands must be washed again.
Contacting the health authorities will be helpful so that the rescuer can be contacted in case that the victim tests positive for COVID-19.
Personal protective equipment in the field of sports: from the ideal to essentialThe minimum personal protective equipment (PPE) which is necessary to protect from droplets and aerosols10 includes medical items requiring a specific and periodical training for its use (e.g., coverall, aprons). It also includes items that are used every day by population since COVID-19 emerged (e.g., surgical or FFP2 masks), which belong to the common first aid kit (e.g., gloves) or could be thus easily incorporated in the first aid kit in sport facilities (e.g., eye protection, FFP3 mask).
It would be necessary to complement sport kits with these items to improve the rescuer's safety when treating a sudden cardiac arrest. In Table 1, the recommended PPE for rescuers from the sports sector is shown, including some items that protect from droplets/aerosols.
Recommendation of Personal Protective Equipment (PPE) for rescuers from the field of sports to prevent the virus transmission by droplets/aerosols.
| Recommended PPE for rescuers from the sports sector |
|---|
| • Gloves• Face mask: preferably protective autofiltering mask (FFP3-N99) [if it is not available, face mask/respirator (FFP2-N95), if not possible, surgical mask].• Eye and Face protection: polycarbonate safety glasses or equivalent, or full-face shield. |
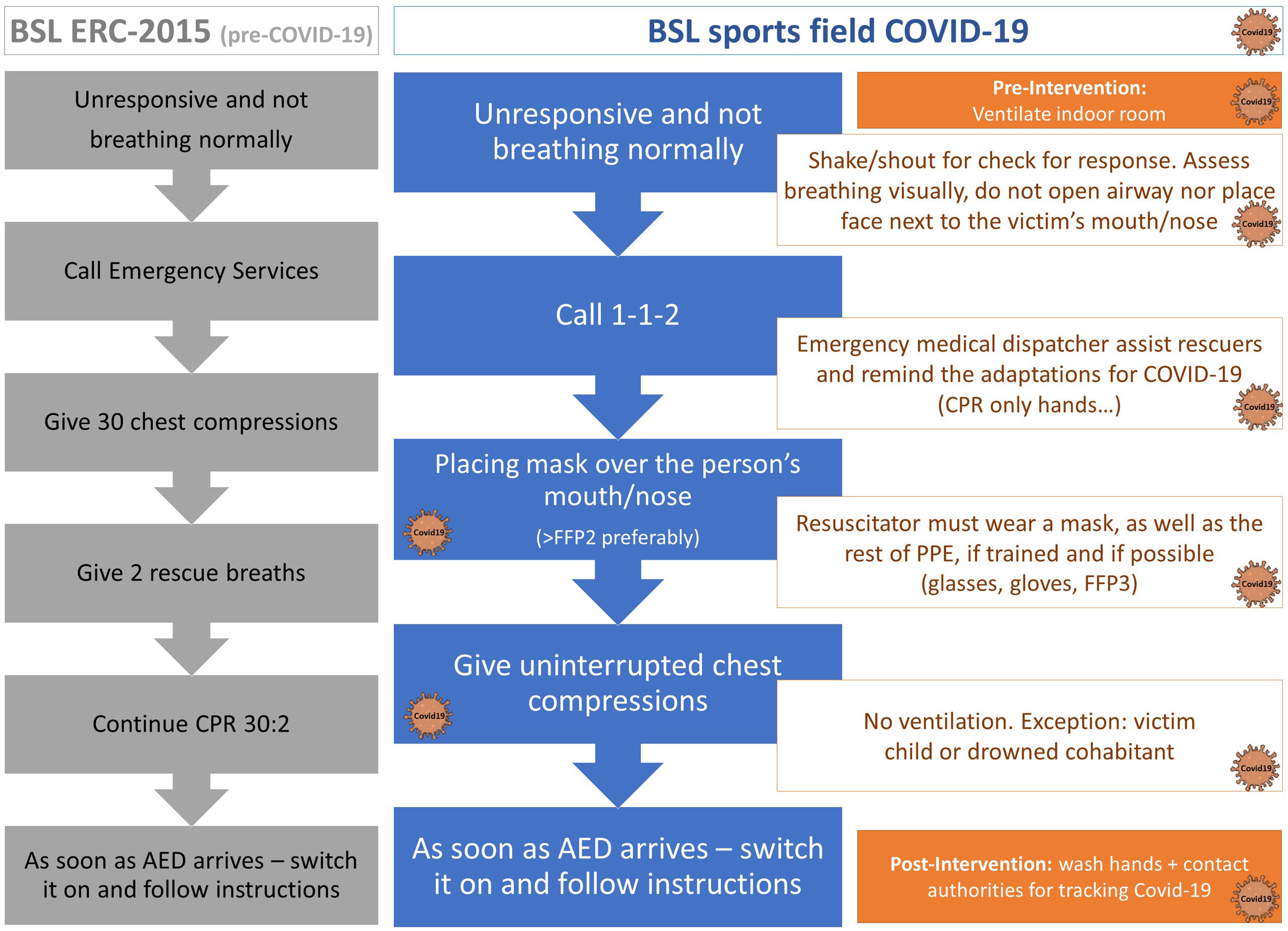
According to the adaptations in BLS (previously explained), in case of out-of-hospital cardiac arrest attended by sports professionals, the current performance protocol of BLS has incorporated some changes in comparison with the 2015 protocol (Fig. 1). On the one hand, the steps of the protocol are different, basically because it has been added that the victim's mouth/nose must be covered and rescue ventilations have been removed (Fig. 1, blue). On the other hand, the skills corresponding to each step have been adapted to ensure the safety of the rescuer (Fig. 1, orange).
Practical implicationsSports professionals may have learnt to perform BLS and use defibrillator while studying or doing other complementary trainings. In fact, after receiving a good quality training in sudden death, this profile of people are able to perform the protocol of BLS and CPR resulting in quality standards above 70% in terms of efectiveness.20 However, skills are lost over time, that is why it is necessary to do refresher trainings.20,21 During the COVID-19 era, trainings and refresher courses that have BLS content for sports professionals should include the adaptations that have been previously explained to ensure rescuer safety. These adaptations affect the procedures before, after and during intervention, in accordance with the new protocol for performance of BLS-AED for sports professionals, the adapted techniques and the use of specific PPE for this collective.
In the same way, not only should sport institutions encourage an update in BLS training for their employees, but they should also complement their first aid kit with equipment to ensure the rescue safety in events of sudden death in their facilities. This includes specific PPE for the sports sector (FFP3 mask preferably, eyes protection and gloves) and a face mask for the victim.
ConclusionBLS training for sports professionals in the COVID-19 era must include adaptations from the protocol for performance, skills and the necessary equipment to ensure the safety of rescuer. The PPE for sports professionals includes equipment that does not require a complex learning and ensures safety against transmission of COVID-19 by droplets/aerosols (FFP3 mask, gloves and safety glasses). The guidelines stated by ERC for lay rescuers can be applied to sports professionals when attending events of sudden death, some complementary adaptations must be taken into account: a face mask must be placed over the victim's mouth/nose before chest compressions, the specific PPE for sports professionals must be worn and performing CPR with ventilations must be considered when the victim is a household member of the rescuer and is suffering an asphyxia-induced cardiac arrest as in the case of a drowning person.
Financial supportSupport received for carrying out the study in the form of grants: no support.
Any part of the manuscript was presented previously in a conference or journal.
Conflict of interestThe authors declare that they don’t have any conflict of interests.