This study aimed to analyze the relationship between the practice of physical activity and the functionality of older people in primary health care, mediated by sedentary behavior.
Material and methodsA cross-sectional study carried out with 654 older people from primary health care in Maringá, Brazil. The International Physical Activity Questionnaire and the World Health Organization Disability Assessment Schedule 2.0 were used. Data analysis was conducted through Structural Equation Modeling (p<.05).
ResultsThe direct effect of sedentary behavior on functionality was weak and significant (β=.10; p<.05). Vigorous activity had a significant (p<.05) and weak (β=−.11) direct effect on sedentary behavior. When mediated by sedentary behavior, the relationship between vigorous activity and functionality showed a weak reduction in the total effect (−.10 to −.09), with an indirect effect of β=.01.
ConclusionsSedentary behavior acts to reduce, weakly, the effect of vigorous activity on the functionality of older people.
Este estudio tuvo como objetivo analizar la relación entre la práctica de la actividad física y la funcionalidad de las personas mayores de la atención primaria de la salud, mediada por el comportamiento sedentario.
Materiales e métodosEstudio transversal realizado con 654 personas mayores de atención primaria de salud en Maringá, Brasil. Se utilizaron el Cuestionario Internacional de Actividad Física y la Clasificación de Discapacidad 2.0 de la Organización Mundial de la Salud. El análisis de los datos se realizó a través del modelado de ecuaciones estructurales (p<0,05).
ResultadosEl efecto directo del comportamiento sedentario sobre la funcionalidad fue débil y significativo (β=0,1; p<0,05). Las actividades vigorosas tuvieron un efecto directo significativo (p<0,05) y débil (β=−0,11) en el comportamiento sedentario. Cuando está mediado por un comportamiento sedentario, la relación entre las actividades vigorosas y la funcionalidad mostró una reducción débil en el efecto total (−0,1 a −0,09), con un efecto indirecto de β=0,01.
ConclusionesEl comportamiento sedentario actúa para reducir, débilmente, el efecto de las actividades vigorosas sobre la funcionalidad de las personas mayors.
Deficiencies and functional limitations in older people are associated with decreased abilities and loss of independence, as well as being risk factors for cardiovascular disease morbidity and mortality.1 About one billion people suffer from deficiency in functionality around the world. Most of these people live in low- or middle-income countries, such as Brazil.2
In addition to this functional decline associated with age,3 the relation with the time of sedentary behavior, which is a major risk factor for disability,4 deficiencies,5 and increased mortality6 are also highlighted.
High levels of sedentary behavior, defined as any activity characterized by an energy expenditure of less than 1.5 METs in sitting or reclining position, are an important risk factor for numerous adverse health outcomes for older people.3 Research in more than 10 countries indicates that older adults are sedentary for approximately 10hours a day.7 Thus, sedentary time management is important for disease prevention and functional improvement,3 and identifying these behaviors can prevent possible diseases through health promotion strategies. Health promotion and physical activity practice can be considered as primary health care tools aimed at integrative and decentralized actions, but they can also be simple actions, in which subjects and collectivities, by self-will and effort, could start practicing it anytime, anywhere, disregarding their life context.8
The literature shows that few older people are involved in the relatively high volume of moderate to vigorous daily physical activity, which seems to be necessary to minimize the adverse effects of sedentary behavior.9 Although engaging in 60minutes a day of moderate-intensity physical activity can compensate for the increased risk and mortality associated with high sitting time, longer total sedentary time can be often associated with fewer sedentary time interruptions.10
Even with some uncertainty, there is a growing understanding that risks associated with prolonged sedentary behavior remain even if individuals meet the recommendations for physical activity.11 This study advances scientifically when it tries to fill a gap in the literature regarding sedentary behavior impact on the functionality and activity of older adults’ users of the primary health care of a Brazilian municipality. Therefore, this study aimed to analyze the relationship between the practice of physical activity and the functionality of older people, mediated by sedentary behavior.
Material and methodsParticipantsAccording to data from the Secretary of Health of Maringá, PR, 42,258 older people attended the Basic Health Units (UBS) of the city in 2016. Considering the population found, the initial sample to be considered was 595 older people, adding 10% of possible losses. The final sample consisted of 654 older people of both gender, considering a 95% confidence level and 4% of margin of error. The software used to obtain the calculations was the StatDisk version 8.4.
The UBSs that older people attended to were subdivided into four regions: East (7 UBS) which covers 21.8% of the population, northern region (8 UBS) with 34.5% of the population, western region (8 UBS) with 23.2% of the population, and south region (8 UBS) that covers 20.4% of the total older population of the city. Knowing the regions composition, three UBSs were selected by lot to be evaluated in each of the regions.
After defining the size of the sample in each region and selecting the UBSs, it was important to maintain the proportion of older people population in the sample, so the calculations to obtain the final sample by UBS according to gender were proportional to the population.
The study included older people of both gender, age 60 years and older, with preserved speech and hearing ability, which allowed the questionnaires to be applied. The Mini Mental State Examination (MMSE) was used to exclude older people with significant cognitive deficits. The MMSE consists of questions grouped into seven categories: temporal orientation, spatial orientation, three-word register, attention and calculation, memorization of the three words, language and visual-constructive capability.12 The cut-off score used by the MMSE for exclusion were: 17 for the illiterate; 22 for the older people with education between 1 and 4 years; 24 for those with schooling between 5 and 8 years; and 26 for those with 9 years or more of schooling. These cut-off scores were based on the criteria of Brucki et al.13 They correspond to the average obtained by these authors for each schooling range, minus one standard deviation. Older people were excluded if classified below the cut-off score specific to their schooling.
InstrumentsTo characterize older people's sociodemographic profile, a semi-structured questionnaire was used consisting of information regarding age (60–69 years, 70–79 years, 80–90 years), gender (male, female), marital status (married or living with a partner, single, divorced, widower), race (white, black, other), the occupational situation (working or not working for own income), monthly income with minimum wage (MW) in 2016 Census of Brazilian Institute of Geography and Statistics (IGBE) as reference (1–2MW, 2.1–3MW, more than 3MW), retirement (yes, no), schooling (did not study, incomplete elementary school, complete elementary education, complete high school, complete higher education).
The functionality has been evaluated by the WHODAS 2.0 instrument. This 12-item instrument covers six domains of disability within 30 days (last month). These domains are: Understanding and Communication (UC), Mobility (MB), Self-Care (SC), Interpersonal Relations (IR), Activity of Daily Living (ADL) and Social Participation (SP). The items are answered on a 5-point Likert scale, which varies from no difficulty (0 points) to the extreme self-reported difficulty (4 points).14
The older people's physical activity level was evaluated using the short version of the International Physical Activity Questionnaire (IPAQ), composed of seven open questions with information that allow to estimate the time spent per week in different dimensions of physical activity (moderate and vigorous physical and walking efforts) and physical inactivity (sitting position). Sedentary behavior was assessed by the last two IPAQ questions: (1) How much time, in total, do you spend sitting on a weekday? (2) How much time, in total, do you spend sitting on a weekend day? The answer is given in hours and minutes. The physical activity data were processed and cleaned according to the protocol indicated by the IPAQ.15,16
ProceduresThis is an analytical, cross-sectional and observational study approved by the Ethics Committee of Human by University Center of Maringá, through opinion number 1.777.797/2016. The data were collected in 12 UBS, of the 33 UBS of Maringá, divided in four regions (north, south, east and west), selected by lot, after authorization of the Permanent Committee for Formation and Training of Health Workers (CECAPS).
Before the beginning of the data collection, a team of 10 researchers was properly trained, and a pilot test was conducted with 30 older people. The volunteers were approached by the researcher in charge or by the research team. They were informed about the justification, objectives and procedures to be carried out, according to guidelines for research with human beings included in Resolution 196/96 of the National Health Council. After these procedures, those who agreed to participate in the research signed the Informed Consent Form (TCLE). The collection was carried out in different days, shifts and schedules, according to the availability of the researchers.
The direct interview was chosen in the application of the questionnaires, due to the possible difficulty of reading, visual problems and comprehension.
Statistical analysisPreliminary analysesPreliminary data analysis was performed using the Kolmogorov–Smirnov normality test. Spearman's correlation (non-parametric) was used to verify the relationship between the variables. Such analyzes were conducted in SPSS v.19.0 software.
Structural Equation Modeling (SEM)The main analysis involved SEM, using AMOS 22.0 software. The hypothetical model verified the existence of five latent factors (Light Activities, Moderate Activities, Vigorous Activities, Sedentary Behavior and Functionality) from the dimensions of the questionnaires. Similar procedures to generate latent variables from the dimensions of the questionnaires have been adopted by several health researchers.17 Thus, the assumptions described in the hypothetical model were tested by SEM, verifying how SB mediates the association between the practice of physical activities and the functionality of older people.
The SEM was tested following the two-step method: (Step 1) Specify and identify the measurement sub-model by performing a confirmatory factor analysis (CFA) of the measurement model and (Step 2) Specify and identify sub-models, establishing paths and errors for endogenous variables.18 The fit quality of the model was analyzed according to the adjustment indices, and the local adjustment was evaluated by the factorial loads and the reliability of the items. The Maximum Likelihood Estimation method was used. The verification of outlier cases was evaluated by Mahalanobis squared distance (D2).19 The univariate distribution was also evaluated by asymmetry (ISkI<3.0) and kurtosis (IKuI<10) and the multivariate distribution (Mardia coefficient of Multivariate Kurtosis).20
The indicators of adequacy of the measurement and structural models (Absolute, Incremental and Parsimonious Adjustments) were: X2 (Chi-square) X2/gl, RMSEA (Root Mean Square Error—less than 0.08), GFI/AGFI (Adjustment Quality Index/Calibrated Adjustment Quality Index—0.90 is considered an acceptable adequacy), CFI (Comparative Adjustment Index, minimum of 0.90), TLI/NFI (Tucker–Lewis Index and Normalized Adjustment Index, minimum of 0.90). The coefficients interpretation of the trajectories had as reference: little effect for factor loads <0.20, medium effect for factor loads up to 0.49, and great effect for factor loads >0.50.20 The significance level adopted was p<0.05.
ResultsPreliminary analysesFrom the 654 patients evaluated, prevailed women (56.0%), married (61.3%), aged between 60 and 69 years (59.2%), monthly income between one and two minimum wages (70.0%), Caucasian (81.0%) and retired (75.0%). It was also observed that most of them had incomplete primary education (43.0%).
Table 1 shows the descriptive values of each study variable, as well as the correlation values between the variables. Sedentary behavior had the following correlations with the functionality: sitting time during the week with functionality in cognition (r=0.15), mobility (r=0.17), self-care (r=0.17), interpersonal relations (r=0.21), and activities of daily living (r=0.29); sitting time at the weekend with minutes of moderate activity a day (r=−0.14), and a week (r=−0.14), with days of vigorous activity (r=−0.22), minutes of vigorous activity a day (r=−0.24) and a week (r=−0.23), with the functionality in cognition (r=0.16), mobility (r=0.16), self-care (r=0.18), interpersonal relations (r=0.21), activities of daily living (r=0.31), and social participation (r=0.14).
Correlation between the variables of sedentary behavior, physical activity practice and functionality.
| Variables | Sedentary behavior | Practice of physical activity | Functionality | ||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | 12 | 13 | 14 | 15 | 16 | 17 | |
| 1. | 0.85* | −0.06 | −0.04 | −0.04 | −0.04 | −0.04 | −0.04 | 0.07 | 0.06 | 0.06 | 0.15* | 0.17* | 0.17* | 0.21* | 0.29* | 0.07 | |
| 2. | −0.11* | −0.05 | −0.04 | −0.11* | −0.14* | −0.14* | −0.22* | −0.24* | −0.23* | 0.16* | 0.16* | 0.18* | 0.21* | 0.31* | 0.14* | ||
| 3. | 0.56* | 0.77* | 0.23* | 0.15* | 0.18* | −0.07 | −0.08 | −0.08 | −0.02 | −0.06 | −0.04 | 0.05 | 0.02 | 0.03 | |||
| 4. | 0.89* | 0.26* | 0.31* | 0.28* | 0.02 | 0.01 | 0.01 | −0.03 | −0.11 | −0.10* | −0.10* | −0.10* | −0.10* | ||||
| 5. | 0.26* | 0.26* | 0.30* | 0.02 | 0.01 | 0.01 | −0.05 | −0.13* | −0.10* | 0.08 | 0.07 | 0.07 | |||||
| 6. | 0.87* | 0.93* | 0.47* | 0.47* | 0.47* | 0.04 | −0.08 | 0.04 | 0.10* | 0.07 | 0.10* | ||||||
| 7. | 0.94* | 0.50* | 0.53* | 0.53* | 0.04 | −0.06 | −0.02 | 0.10* | 0.10* | 0.13* | |||||||
| 8. | 0.51* | 0.53* | 0.53* | 0.02 | −0.10* | 0.01 | 0.10* | 0.08 | −0.13* | ||||||||
| 9. | 0.98* | 0.99* | −0.05 | −0.14* | −0.02 | 0.03 | −0.03 | −0.04 | |||||||||
| 10. | 0.99* | −0.06 | −0.13* | 0.03 | 0.02 | −0.02 | −0.03 | ||||||||||
| 11. | −0.06 | −0.13* | −0.03 | 0.02 | −0.03 | −0.03 | |||||||||||
| 12. | 0.63* | 0.39* | 0.41* | 0.60* | 0.56* | ||||||||||||
| 13. | 0.34* | 0.29* | 0.68* | 0.59* | |||||||||||||
| 14. | 0.19* | 0.38* | 0.28* | ||||||||||||||
| 15. | 0.42* | 0.34* | |||||||||||||||
| 16. | 0.56* | ||||||||||||||||
| 17. | |||||||||||||||||
| x | 300.0 | 396.9 | 3.9 | 76.3 | 390.5 | 2.0 | 40.6 | 128.8 | 0.4 | 23.4 | 40.4 | 0.9 | 1.7 | 0.2 | 0.4 | 1.0 | 1.2 |
| dp | 210.8 | 342.9 | 3.3 | 70.5 | 358.6 | 3.9 | 71.4 | 291.4 | 0.8 | 69.1 | 170.3 | 1.2 | 1.8 | 0.7 | 0.8 | 1.2 | 1.4 |
In bold are the significant correlation between variables of sedentary behavior, physical activity practice and functionality.
Significant correlation—p<0.05. Note: 1. Sitting time during the week; 2. Sitting time during the weekend; 3. Hike days; 4. Min. walk per day; 5. Min. walk per week; 6. Days of moderate activity; 7. Minutes of moderate activity per day; 8. Minutes of moderate activity per week; 9. Days of vigorous activity; 10. Minutes of vigorous activity per day; 11. Minutes of vigorous activity per week; 12. Functionality in cognition; 13. Functionality in mobility; 14. Functionality in self-care; 15. Functionality in interpersonal relationships; 16. Functionality in the activities of daily living; 17. Functionality in social participation.
The minutes of walking a day are related with self-care functionality (r=−0.10), interpersonal relations (r=−0.10), activities of daily living (r=−0.10), and social participation. Minutes of walk per week with mobility functionality (r=−0.13) and self-care (r=−0.10). Days of moderate activity per week with functionality in interpersonal relations (r=0.10) and in social participation (r=0.10). Minutes of moderate activity per day with functionality in interpersonal relations (r=0.10), activities of in daily living (r=0.10) and in social participation (r=0.10). Minutes of moderate activity per week with functionality in mobility (r=−0.10), in interpersonal relations (r=0.10) and in social participation (r=−0.13). Finally, the days of vigorous activity per week, minutes of vigorous activity per day and per week related with functionality in mobility (r=−0.14/r=−0.13/r=−0.13, respectively).
Structural Equation Modeling (SEM)Initially, the measurement models of the five latent variables (Step 1 of the SEM) were tested, verifying the relationships of the observed items in their respective factors by CFA. All sub-models presented adequate adjustment indices and the quality of the local adjustment. The internal reliability of the items were also confirmed, since all trajectories presented significant factorial loads (p<0.05), greater than 0.50. These results confirm the latent models and allow the test of the structural equations model (Step 2).
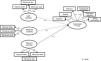
A model was tested for trainers without SB mediation, with direct trajectories between practice of physical activity and functionality (M1). This model did not present adequate adjustment indicators [X2(87)=1161.66; p=0.001; X2/gl=13.352; CFI=0.084; GFI=0.83; AGFI=0.77; NFI=0.83; TLI=0.80; RMSEA=0.14; P (rmsea<0.05)=0.0.001, explaining only 2% of the functionality variance (Fig. 1). In addition, the trajectories of light (β=−0.03) and moderate (β=0.03) activities for the functionality were not significant (p>0.05). Therefore, these two latent variables were deleted, and the model was tested again.
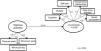
The second model (M2) without the latent variables of light and moderate activities presented an acceptable fit [X2(26)=118.46; p=0.001; X2/gl=3.556; CFI=0.97; GFI=0.96; AGFI=0.94; NFI=0.96; TLI=0.95; RMSEA=0.07; P (rmsea<0.05)=0.002] but explaining only 1% of the functionality variance (Fig. 2). The trajectory of the vigorous activities had a significant (p=0.028) and weak (β=−0.11) effect, indicating that each increase of 1 standard deviation in the vigorous activity unit had a reduction of 0.11 standard deviation in the unit of functionality. This finding indicates that the practice of vigorous activities is associated with a poor improvement in functionality.
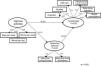
In the third model (M3), SB was inserted as a mediator variable of the effect of vigorous physical activities practice on functionality. The M3 represents several hypothetical relations of association between the variables, and these magnitudes are described by the direct and indirect effects. The model (M3) provided acceptable adjustment values [X2(38)=165.54; p=0.001; X2/gl=3.36; CFI=0.96; GFI=0.96; AGFI=0.92; NFI=0.96; TLI=0.95; RMSEA=0.07; P (rmsea<0.05)=0.001] (Fig. 3).
The latent functionality variable is explained in only 3% by the structural model (Vigorous Activities+Sedentary Behavior), while RTA is explained in only 1% by Vigorous Activities (Fig. 3). In the direct relationship established between Vigorous Activities and Functionality, the effect is significantly positive and weak (β=−0.10, p<0.05) (for each increase of 1 standard deviation of the Vigorous Activities Practice, Functionality decreases by 0.10 standard deviations), that is, the greater the practice of Vigorous Activities, the better the functionality. Regarding sedentary behavior, the direct effect on the Functionality was weak and significant (β=0.10, p<0.05) (for each increase of 1 standard deviation of the sedentary behavior, the Functionality increases by 0.10 standard deviations), that is, the longer the sedentary behavior, the worse the functionality. In addition, vigorous activities had a significant (p<0.05) and weak (β=−0.11) direct effect on sedentary behavior (Table 2).
When mediated by sedentary behavior, the relationship between Vigorous Activities and Functionality showed a weak reduction in the total effect (−0.10 to −0.09), with an indirect effect of β=0.01 (Table 2). Thus, it is evident that although sedentary behavior acts to reduce the effect of vigorous activities on functionality, this moderating/damaging effect is very weak, indicating that if older people practice vigorous activities their functionality will have a slight improvement, regardless of the time of sedentary behavior.
DiscussionThis study aimed to analyze the effect of physical activity on the functionality of older people in primary health care mediated by sedentary behavior. There are no similar studies regarding Brazilian older people users of primary health care, even more so in a region of northwest Paraná.
The main findings of this study indicate that the more vigorous the physical activities older people perform, the better their functionality, but this relation was weak, as well as the finding that sedentary behavior acts also reducing the effect of vigorous activities on the functionality of older people users of primary health care. However, the results may be affected by the fact of using a tool measuring functionality that is not objective.
Regarding the practice of vigorous activities, it is associated with a poor improvement in functionality (Fig. 2). It can be explained by the fact that functionality covers not only the capacity/ease to perform motor activities (e.g. shift), but also cognition, social participation, interaction with people, which is not necessarily related to the intensity of the physical activity performed, reported by older people. It is known that aerobic exercise and muscle strength, performed at higher intensities, can improve functional capacity.21–23
Note that World Health Organization guidelines24 recommend that older adults participate in at least 150minutes of moderate to vigorous physical activity per week in periods of at least 10minutes. However, in our study, we found that performing these vigorous activities weakly improves the functionality of older people in primary care.
It was found that the longer the sedentary behavior, the worse the functionality (Fig. 3). This agrees with Bertolini et al.,25 who report that aging associated with sedentary behavior increases functionality decline, since it decreases neuromotor functions, making the individual weaker and increasing risks, such as falls, fractures, noncommunicable chronic diseases, among other disabilities. And with compromised functionality, individuals tend to lose independence to perform activities of daily living.26 As well as in a prospective cohort study with 61,609 older women in a 12-year follow-up which observed that, in comparison to the older women who reported sedentary expenditure of ≤6h/day, those with longer sedentary period had lower physical condition to perform daily activities.27
In our study, we used the WHODAS 2.0 instrument to evaluate the functionality, covering its several domains, and not only the ability to perform activities of daily living. Other studies also found an association between sedentary behavior and low functionality, but with the use of different tests and physical capacities.28,29 One of the factors that may explain this relationship is that the sitting or reclining posture, used in sedentary behavior, does not require muscle contraction and joint lubrication, and, consequently, older people do not receive stimuli for increased joint muscle mass and quality. Another explanation for this result may be related to the occupation of older people, mostly retired (75%), which, therefore, did not have to go to work.
It was evident that if older people practiced vigorous physical activities, their functionality would only slightly improve, regardless of the time of sedentary behavior, which highlights its significance in older people's lives. In short, although older people are physically active, performing more intense activities, such behavior may not compensate for the adverse effects of prolonged time in sitting position.
Studies11,30 showed that, regardless of the physical activity (type, intensity, volume), shortening the time spending on sedentary behavior and increasing the number of sedentary time intervals may have a positive effect on health outcomes. According to Loprinzi,31 sedentary behavior is associated with multi-morbidity independent of light physical activity and adhesion of moderate/vigorous physical activity guidelines, highlighting the importance of minimizing prolonged sedentary behavior. For White et al.,32 the appropriate time and intensity of physical activity practice does not exclude the risk, for example, of mortality due to excess of sedentary activities.
When the correlations between some of the studied variables were identified (Table 1), it was observed that the longer the seated/reclined time in the weekend, the lower the minutes of moderate activity performed per day and week, as well as the fewer the days of vigorous activity. Alves et al.,33 report that, over the years, the levels of physical activity in the population decrease and the time in sedentary activities, such as sitting, increases. The causes for such behaviors may be the absence of environmental stimulation of healthy habits; the increasingly easy access to technological instruments, such as electronic devices that provide more sedentary behavior during leisure time, biological factors and age.
Table 1 also shows that walking is associated with better functionality related to self-care, interpersonal relationships, daily living activities and social participation. Costa et al.,34 and Inácio et al.,35 suggest that walking is the most common activity reported by older adults.
The strengths of the study were: representativeness of the MMSE sample use as an inclusion criterion of the subjects; assessment of sedentary behavior based on total sitting time, and not just on time spent watching television. On the other hand, the cross-sectional design of the study, which does not allow a cause-and-effect relationship, and self-report time-based assessment can be considered as limitations, although this strategy has been used in other population-based studies.36 In addition, the instruments used to assess physical activity and functionality were self-reported, which may generate some bias. A last limitation is that the sample is a fairly young elderly population (the vast majority are in the 60–69 age group) and this may affect the results, since younger elderly tend to be more physically active than older elderly.
Considering the results obtained and presented, it is concluded that the relationship between the intense physical activities performance and the functionality of older people in primary health care is weak, as well as the fact that sedentary behavior decreases the effect of vigorous activities on the functionality of these older adults.
In this sense, it is necessary to further track this type of behavior and the adoption of individual and collective counseling actions for UBS users, mainly in primary health care, in order to prevent the possible damages caused by the excessive time spent in sedentary activities.
Conflict of interestsThe authors declare that they have no conflict of interests regarding the publication of this paper.
The Permanent Training and Training Office of the health workers of the municipality of Maringá, Paraná, Brazil.