Anterior Cruciate Ligament (ACL) injuries stand out as the most severe in sports such as soccer. This study presents the rehabilitation process of a professional soccer player who suffered a total ACL tear. It details the treatment performed after the surgical intervention and all the adaptations that had to be applied in the rehabilitation process due to the lockdown period established at the beginning of the COVID-19 pandemic. During the period comprised between weeks 9 and 21 post-surgery, the rehabilitation treatment was carried out virtually, adapting the actions, work environment and equipment used. Despite the limitations it entailed, the virtual format and the adaptations in the treatment allowed the rehabilitation process to continue, fulfilling all the pre-established objectives and deadlines with a consequent satisfactory and safe return to competitive sport. After carrying out a bibliographic research, no clinical cases have been found regarding the adaptation of the rehabilitation process of an ACL reconstruction in a professional soccer player during the COVID-19 lockdown.
Anterior Cruciate Ligament (ACL) injuries are considered one of the most severe injuries in soccer, 1 causing in many cases a long period of sport inactivity.2,3 The incidence is higher in people who practices sports such as soccer, that include actions classified as non-contact,2,4 such as the changes of direction or pivoting manoeuvres.5,6 Numerous studies have focused the investigation on ACL injuries in professional soccer players, the rehabilitation process and the Return to Sport (RTS).6
Due to the COVID-19 (SARS-CoV-2) pandemic, on March 14th 2020 the state of alarm was declared in Spain and lockdown measures were applied to the population.7
This paper describes the case of a professional soccer player of the Greece Super League 1 and details the process of rehabilitation after suffering a total tear and reconstruction of the ACL. Due to the lockdown, between March 14th and June 21st,2020, the treatment was established in a virtual format, which led to the adaptation of the workout, the work environment and the material used.
Case descriptionProfessional soccer player, midfielder (age, 29 years old; height, 1,75m; weight, 70Kg), who suffered a total right knee ACL tear during a soccer match of the Greek Super League 2019-2020 season, in a pivoting action. On December 26th, 2019, was submitted to a surgical reconstruction of the ACL with a patellar tendon self-grafting.
The rehabilitation program started in his club, and on February 17th, 2020, the player travelled to Barcelona in order to start the treatment at Invisible Training. In the initial physical examination, there was evidence of swelling, signs of joint effusion and an increase in the surface temperature. In relation to the Range of Motion (ROM) there was a deficit of the knee flexion (105°). The tibio-femoral rotations and the knee extension ROM values where in normative ranges. Regarding muscular balance, with an assessment by manual resistance it denoted a deficit of strength of the main muscular groups: quadriceps, hamstrings, glutes, adductors, and the triceps surae.
The treatment consisted of three stages, comprised between the 9th and 21st week post-surgery, which were influenced by the social and sanitary circumstances of the moment (Table 1). Until the 12th week, daily physiotherapy treatment was accomplished in the centre.
Treatment carried out according to the week post-surgery and the adaptations to lockdown.
AROM (Active Range of Motion), B. (Bilateral), COD (Change of Direction), CONC. (Concentric), CKC (Closed Kinetic Chain), DF (Diacutaneous Fibrolisis), ECC (Eccentric), Ex. (Exercises), EXT. (Extension), FLEX. (Flexion), FWB (Full Weight Bearing), ISOM. (Isometric), Man. Ther. (Manual Therapy). min. (minutes), Mo. (Mobility), Mobs. (Mobilization), MR (Manual Resistance), OKC (Open Kinetic Chain), PRO (Pronation), PROM (Passive Range of Motion), PT (Physical Therapist), Reps. (Repetitions), ROM (Range of Motion), Rot. (Rotations), SIT (Sitting), ST (Standing), SUP. (Supination), UNI (Unilateral), WB (Weight Bearing).
Due to the confinement, from the 13th to the 19th week, a new therapeutic plan was established aiming to adapt the treatment to a virtual format and the necessary material was provided. From the 19th to the 21st week, the face-to-face treatment was restored. In this last stage, strength, structural and functional tests (Table 2) were added to the treatment in order to objectify possible inter-limb asymmetries and determine objectively if the player was ready for the RTS. From the 21st week onwards, the player returned to his club of origin for the last period of the readaptation and RTS. On June 27th, 2021 (26 weeks post-surgery), he received the sport discharge and played an official competitive game with a satisfactory RTS.
Strength, structural and functional tests.
The main objectives and interventions performed in the continuum of the rehabilitation process until the RTS in ACL injuries have been detailed by numerous authors.2,8 Nevertheless, after carrying out a bibliographic research, no similar cases describing the process of rehabilitation and follow-up in a virtual format of an ACL injury in a professional soccer player during the lockdown period have been found.
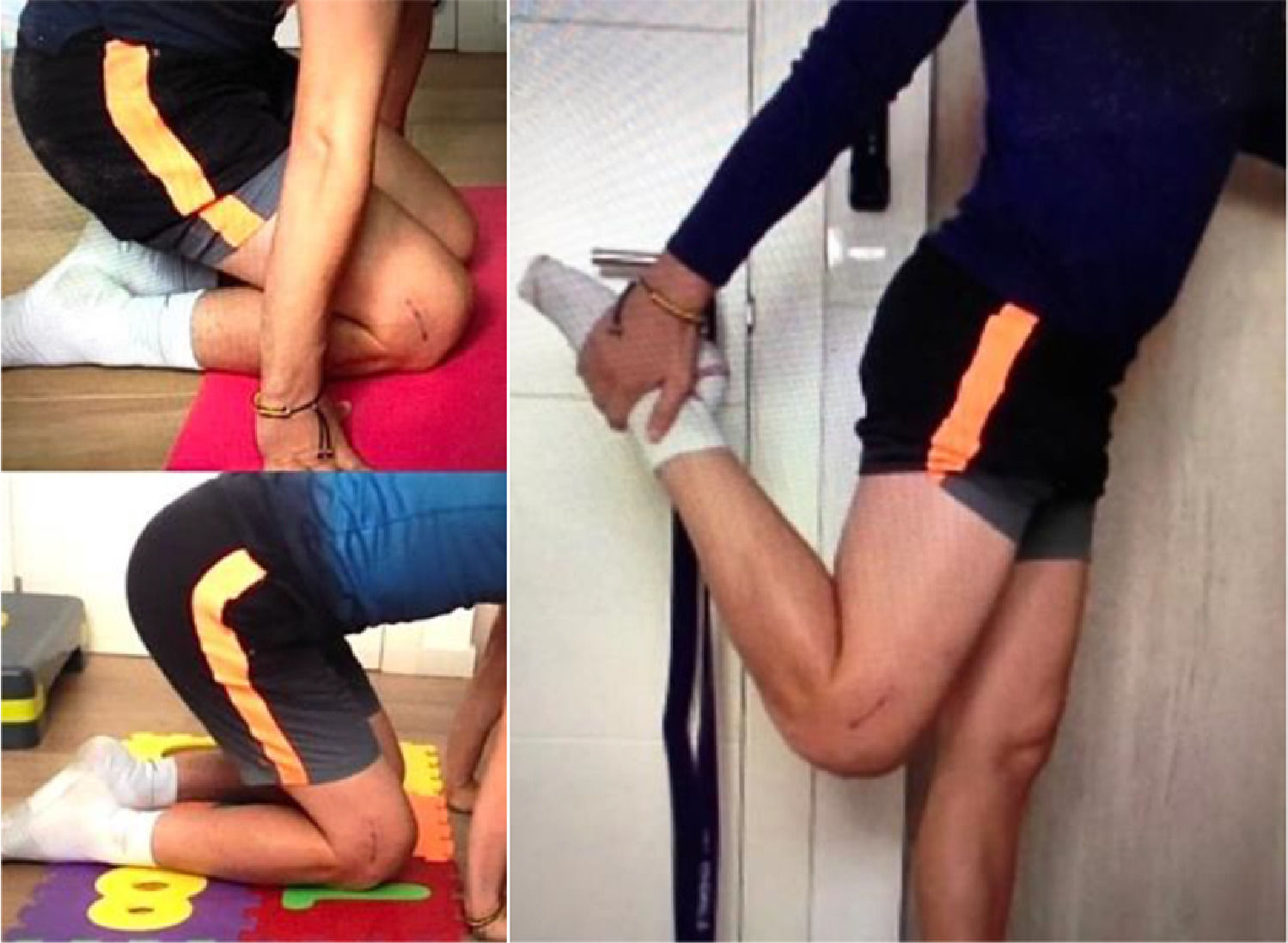
Strategies to restore the ROM of the patella and knee, and for the control of the post-surgery oedema and inflammation have been previously described.9,10 During the lockdown, the treatment adaptations allowed the accomplishment of the objectives established for a satisfactory recovery (Fig. 1).
To restore the levels of quadriceps and hamstrings strength with symmetric values in the functional strength assessment is essential for a safe RTS and reduce the risk of re-injury.8,10,11 The schedule of tasks and the control of loads by the physiotherapists, with the supervision of a correct execution in the daily virtual follow-up, allowed the progression and achievement of strength values in relation to the contralateral leg.
Although the lockdown could have involved in a larger inactivity period, it has been possible to objectify that with the adaptation to the virtual format and the availability of proper material at home, the objectives can be achieved within the pre-established deadlines, allowing a competitive RTS, in a safe manner and similar to other cases described with a face-to-face follow-up.6,12
This study demonstrates that satisfactory results can be obtained with inexpensive material, added to the professional's knowledge and skills. Also, it is questioned whether the face-to-face intervention of the physiotherapist is strictly necessary or if, on the other hand, with supervision and an adequate method and approach by the professionals, the objectives can also be successfully achieved.
ConclusionThe virtual format and the treatment adaptations, with a load control, a correct supervision of the execution of the workout and a progressive approach of the tasks by the physiotherapists, demonstrate that all objectives can be accomplished in the pre-established deadlines after an ACL tear and its surgical reconstruction, with the consequent safe and satisfactory RTS.
FundingThis research received no external funding.